Main Menu
- EnvironmentLABORATORIA
Main Menu
- EnvironmentLABORATORIA
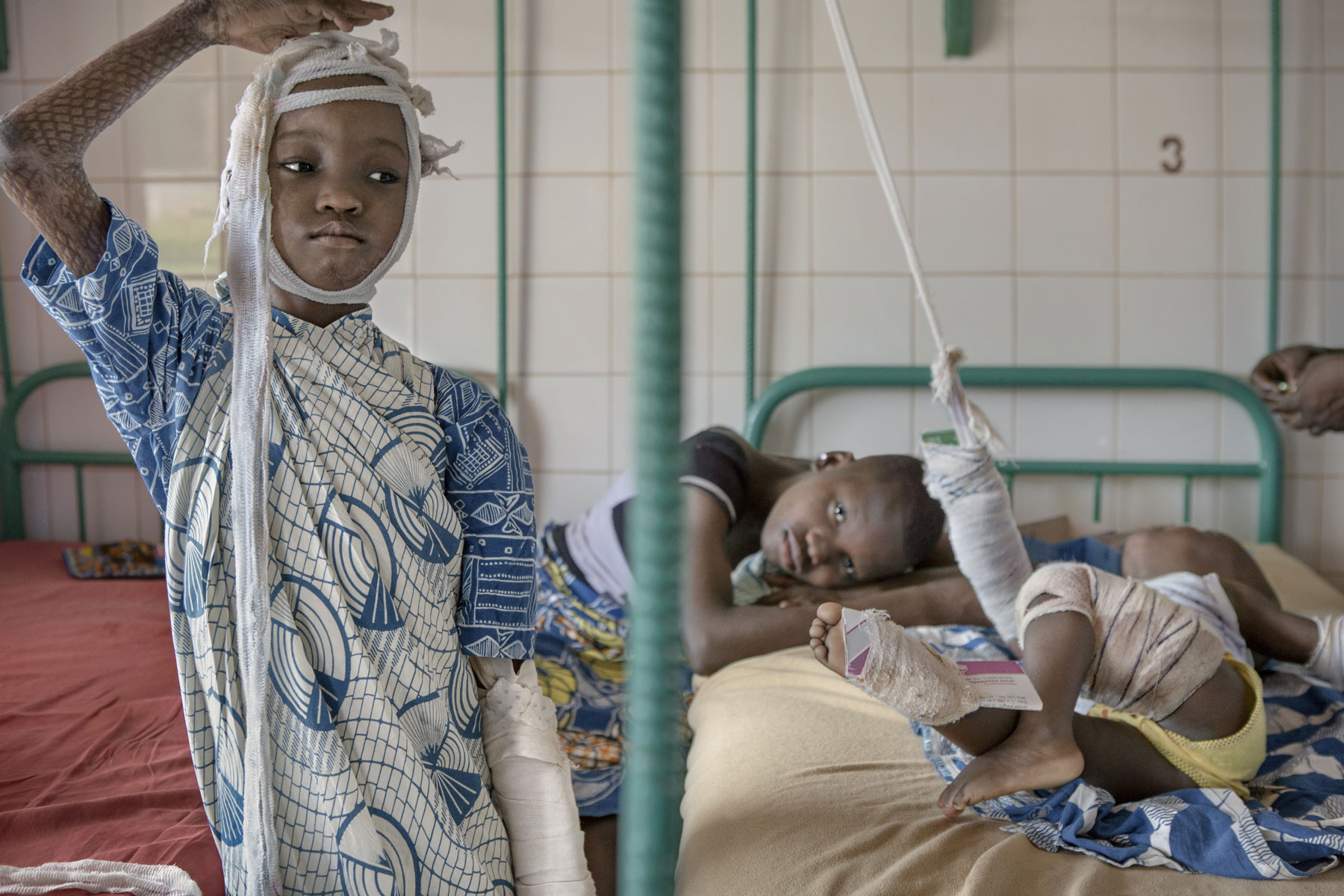
Freud Lokossou, aged eight, dressed up in a straw costume on new year’s eve and another child set fire to him. He has been in Gbenmontin Hospital for seven months.

Freud Lokossou, aged eight, dressed up in a straw costume on new year’s eve and another child set fire to him. He has been in Gbenmontin Hospital for seven months.
“Africa under your skin” documents the daily life of the doctors and patients in hospitals, clinics, maternity wards, rehabilitation centers, emergency rooms and awareness sessions in communities, affected by Buruli ulcer in Benin.
Benin, with almost ten million inhabitants and which ranks 165 out of 187 in the Human Development Index (2022 data), is one of the countries most rife with Buruli ulcer in the world.
* The project is supported by Fundación Anesvad.
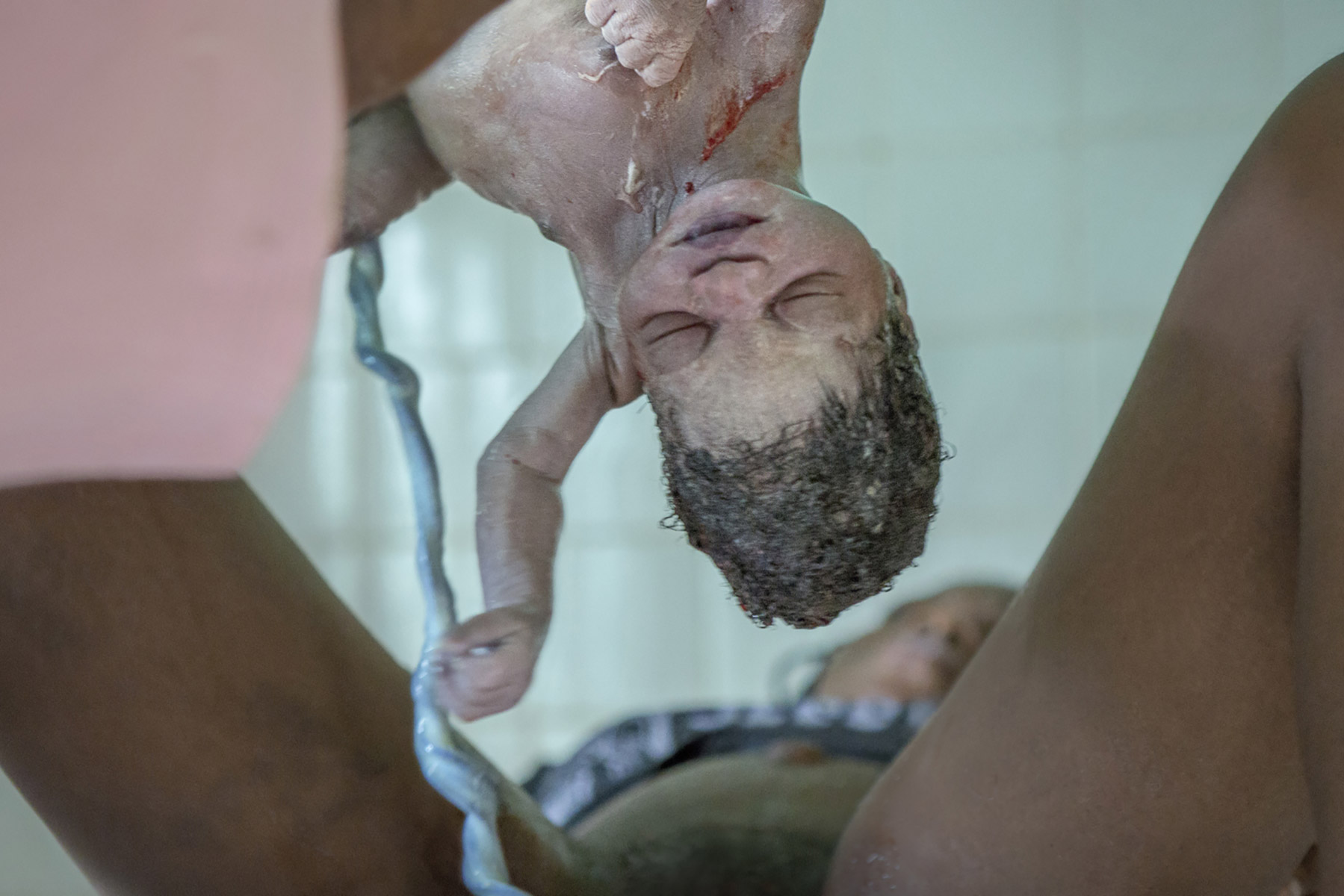
Odou has just come into the world in a maternity hospital in Sedjne Denou, Benin. When this first-time mother sees her baby for the first time she exclaims, relieved “Thank you Jesus for making everything go well”. A few minutes after the birth, she has to lie on the floor because there are not enough beds. In Benin, 56 in every thousand children born alive and 405 in 100,000 women die in childbirth. Added to these premature deaths are those caused by a lack of healthcare and, in many cases, diseases that are no longer lethal in many other regions of the world.
Buruli ulcer, known as the “mysterious disease” because its causes are still unknown, is a neglected tropical disease of the same family as leprosy and tuberculosis, which destroys the skin and soft tissues causing large ulcers on arms and legs.
Fundación Anesvad, whose motto is “for the right to health”, decided to answer this urgent call and has been present in the country since 2002.Their support has evolved from prompt attention to those affected by the disease to a more integral strategy which comprises prevention – informing the communities on how to avoid and identify the disease – attention to maternal-infant health, guaranteed access to services in the area of sexual and reproductive health, guaranty of correct nutrition for patients in the different health centers, reinforcement of basic hygiene and sanitation in the most affected areas, etc.
A holistic vision which has translated the promotion of the right to health to a net reduction in the mortality associated with Buruli ulcer and the improvement of certain indicators in the health of mothers and children under the age of five.
These efforts have even shown results in the area of gender equality and the autonomy of women.
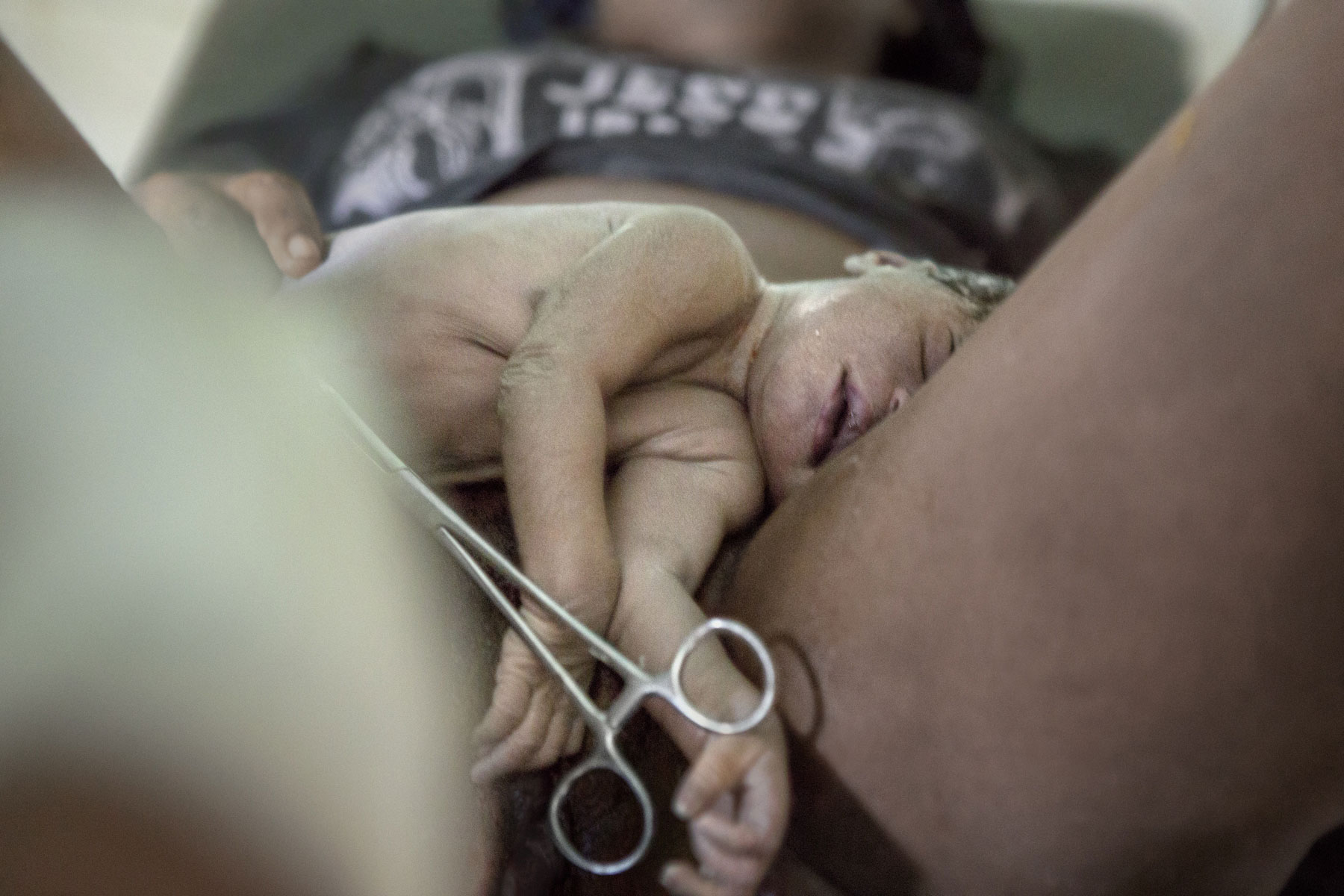
Odou rests on her mother’s belly while they wait for a health worker to finish cutting the umbilical cord. Both are healthy. Both are fortunate in spite of a lack of resources and hospital staff. Benin is a small country with a population of around 10 million. Half the population lives in rural areas and 48 percent live on less than $1,25 a day. Underdevelopment, poverty and disease make it impossible for much of the population to access basic health services.

Odou, alive for just minutes, waits in a cot for a first check-up by medical staff at the maternity hospital. From now on her chances of seeing her fifth birthday will depend on whether she can survive diarrhoea, malnutrition, malaria, mother-to-child HIV transmission and all kinds of other diseases. Five million children die in Africa each year from treatable and curable illnesses, that’s 14,000 every day. Humanitarian organization “Save the Children” laments the situation, saying “the unfair lottery of birth violates every child’s right to an equal start in life”.

Odou, alive for just minutes, waits in a cot for a first check-up by medical staff at the maternity hospital. From now on her chances of seeing her fifth birthday will depend on whether she can survive diarrhoea, malnutrition, malaria, mother-to-child HIV transmission and all kinds of other diseases. Five million children die in Africa each year from treatable and curable illnesses, that’s 14,000 every day. Humanitarian organization “Save the Children” laments the situation, saying “the unfair lottery of birth violates every child’s right to an equal start in life”.

Mother and new born enjoy their first moments together at a hospital in Tohues. The fertility rate in Benin is five children per woman, the first at age 20. Every year, 36 children are born per 1000 inhabitants and the population is growing at a rate of 2.78. Life expectancy in Benin has increased considerably in recent decades thanks to better healthcare and access to services. Fifty years ago it was less than 45 years, whereas now it is more than 60.
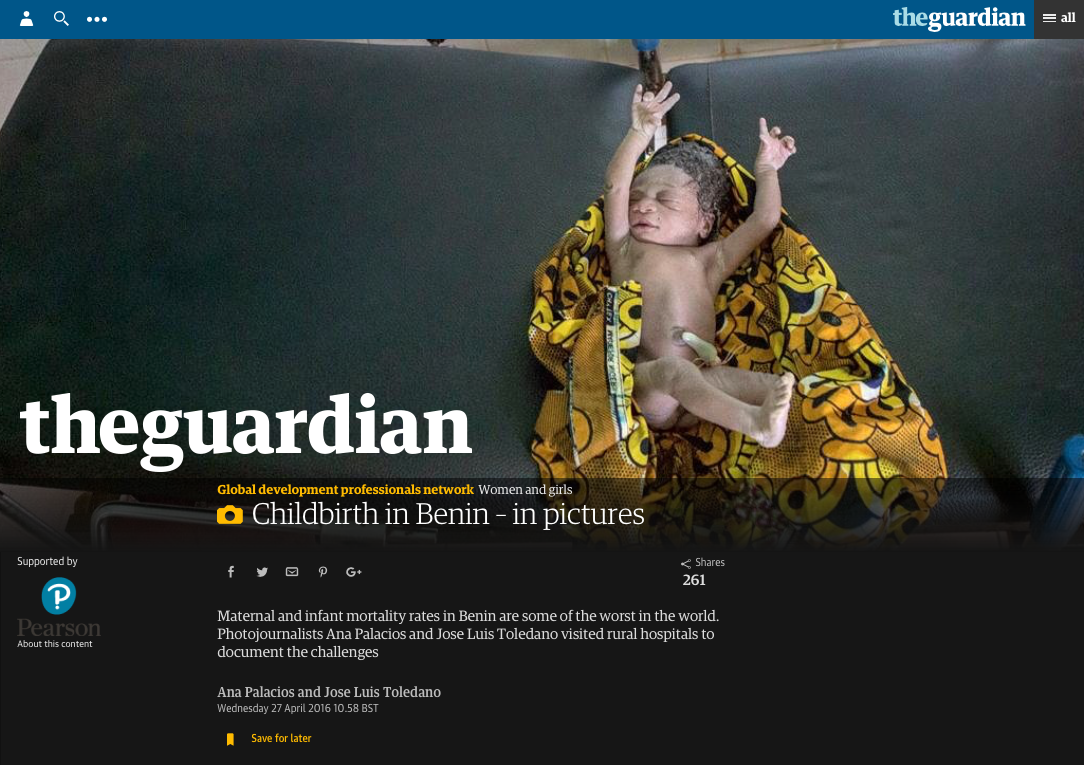
The Guardian – Childbirth in Benin – in pictures. April 27th, 2015.

Babies have a weigh-in at the hospital in Gbemontin, Benin. Many of the children who come to this hospital suffer from varying degrees of malnutrition. Child malnutrition is another cause of death and affects more than 20 million children in the world. Millions more suffer from physical and mental disabilities caused by a deficient diet. In Benin, this affects 20 per cent of children up to the age of five years. Malnourishment among pregnant women means that 15 per cent of children are born underweight.

Babies have a weigh-in at the hospital in Gbemontin, Benin. Many of the children who come to this hospital suffer from varying degrees of malnutrition. Child malnutrition is another cause of death and affects more than 20 million children in the world. Millions more suffer from physical and mental disabilities caused by a deficient diet. In Benin, this affects 20 per cent of children up to the age of five years. Malnourishment among pregnant women means that 15 per cent of children are born underweight.



Tiempo – La lotería de nacer en África (The lottery of being born in Africa). July 2016
Africa’s skin. Treatment.
First step: prevention.
Final step: reinsertion
The disease began spreading at an alarming rate towards the end of the 20th Century. In 2004 the WHO decided to intervene by adopting a resolution aimed at increasing surveillance of Buruli ulcer and promoting research. The disease continued to spread geographically, with sufferers now recorded in more than 30 countries across Africa, Asia and the Western Pacific, prompting the WHO to issue a new alert in 2013. A new resolution was adopted, calling member states to step in and put measures in place to improve the health and social welfare of population groups affected by Neglected Tropical Diseases.
After awareness raising comes prevention, treatment (with or without surgery) and rehabilitation, followed by reinsertion at the very end of the disease process. The hospital monitors patients whose treatment has been completed to supervise their progress and ensure there are no new sources of infection.
Photography and video
Ana Palacios
With the collaboration of
DKV Health Insurance and Anesvad

The waiting area at Gbemontin Hospital in Benin, where 40,000 people were treated in outpatient clinics in 2014.
In Benin, home of voodoo, there’s a strong tradition of going to traditional witch doctors and shamans when someone gets sick. But Gbemontin Hospital is getting more visitors year after year, and it’s brimming with patients who see Sister Julia Aguiar as some sort of mystical skin guru. Last year, this “dispensary”, as the facility is referred to in the Benin registry, treated more than five thousand people and carried out over 40,000 medical consultations, a reasonably high figure in a country with 10 million inhabitants.



Days Japan – Inequality is Skin Deep. April 1st, 2016
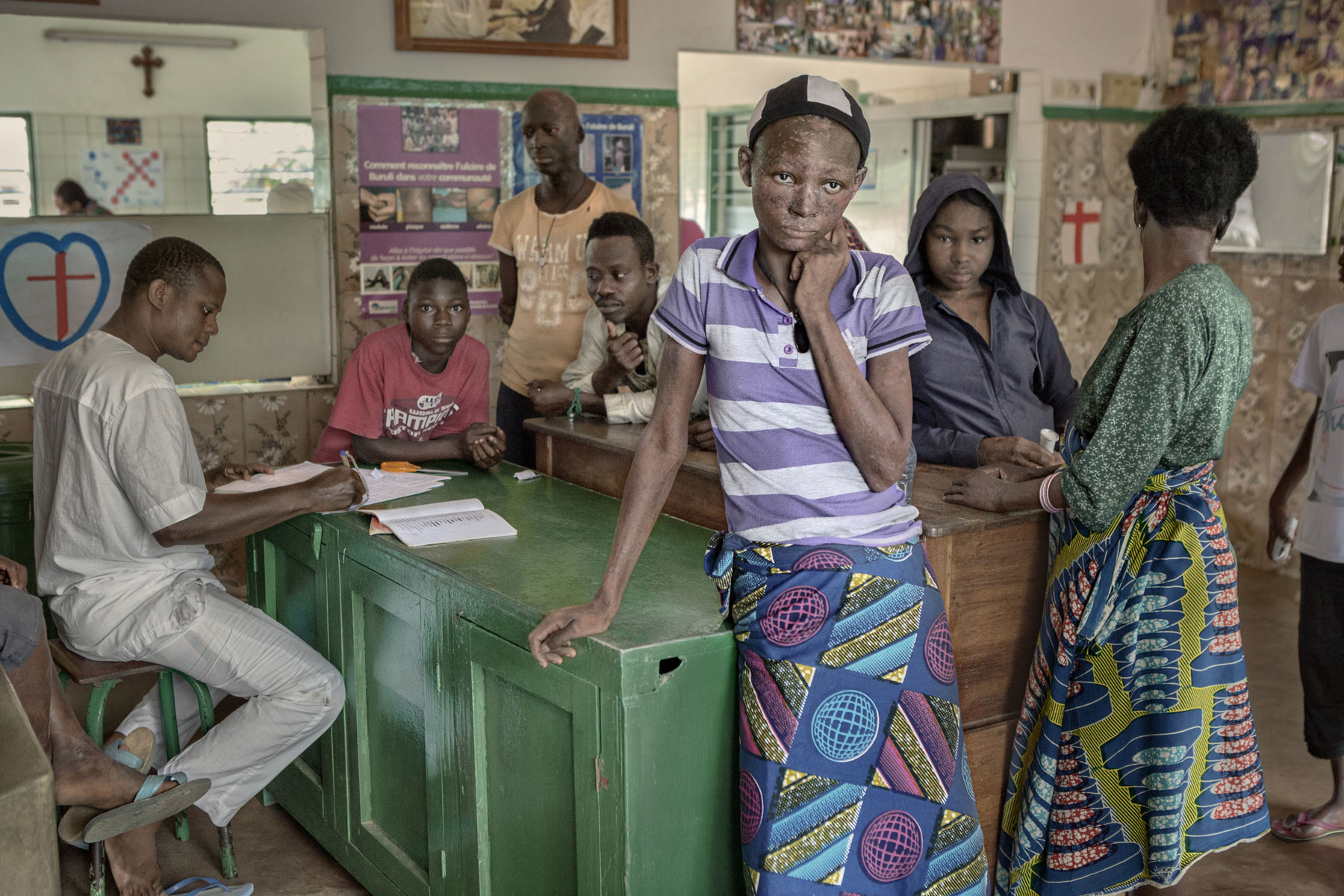
Patients from the Davougon former leper colony wait to get their meal vouchers. It’s part of a nutrition project run by Spanish NGO Anesvad, which has been in Africa fighting buruli ulcer and other neglected tropical diseases for seventeen years.

Three-year old Ossou Delphine waits with her mother Alice in the maternity ward at Sedje Denou to have more treatment for the ulcer on her right arm.

Three-year old Ossou Delphine waits with her mother Alice in the maternity ward at Sedje Denou to have more treatment for the ulcer on her right arm.
Africa’s skin. Treatment.
Photography and video
Ana Palacios
With the collaboration of
DKV Health Insurance and Anesvad
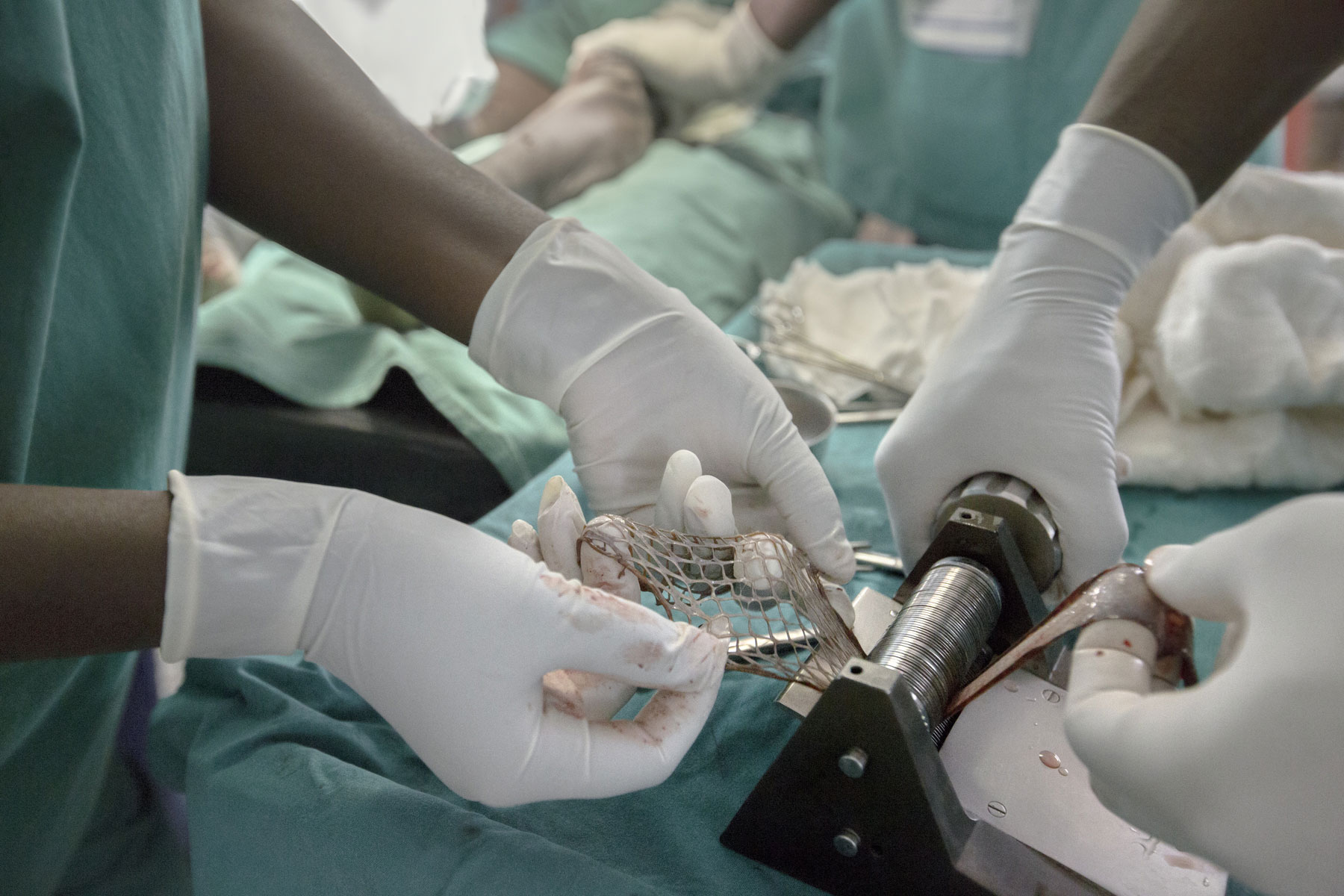
This surgical instrument is a skin graft mesher. It cuts skin for grafting, turning the epidermis into a mesh that enables a larger surface area to be covered during the operation. It produces “snakeskin effect” scars. The technique is manual and rudimentary and needs no electricity, which is crucial in rural african hospitals where the power supply is often unreliable.
Like snakeskin. That’s how your skin looks, with a kind of diamond pattern, when you have a skin graft done in Africa. That’s if you’re lucky and they have the little stretching machine that makes holes in the skin cut from you so it can then be stretched like a mesh over the wound, like one of those string shopping bags. Otherwise, after the operation when they use strips of your healthy skin to cover the diseased patches, it can look like a bar code has been hand drawn all over your thigh.
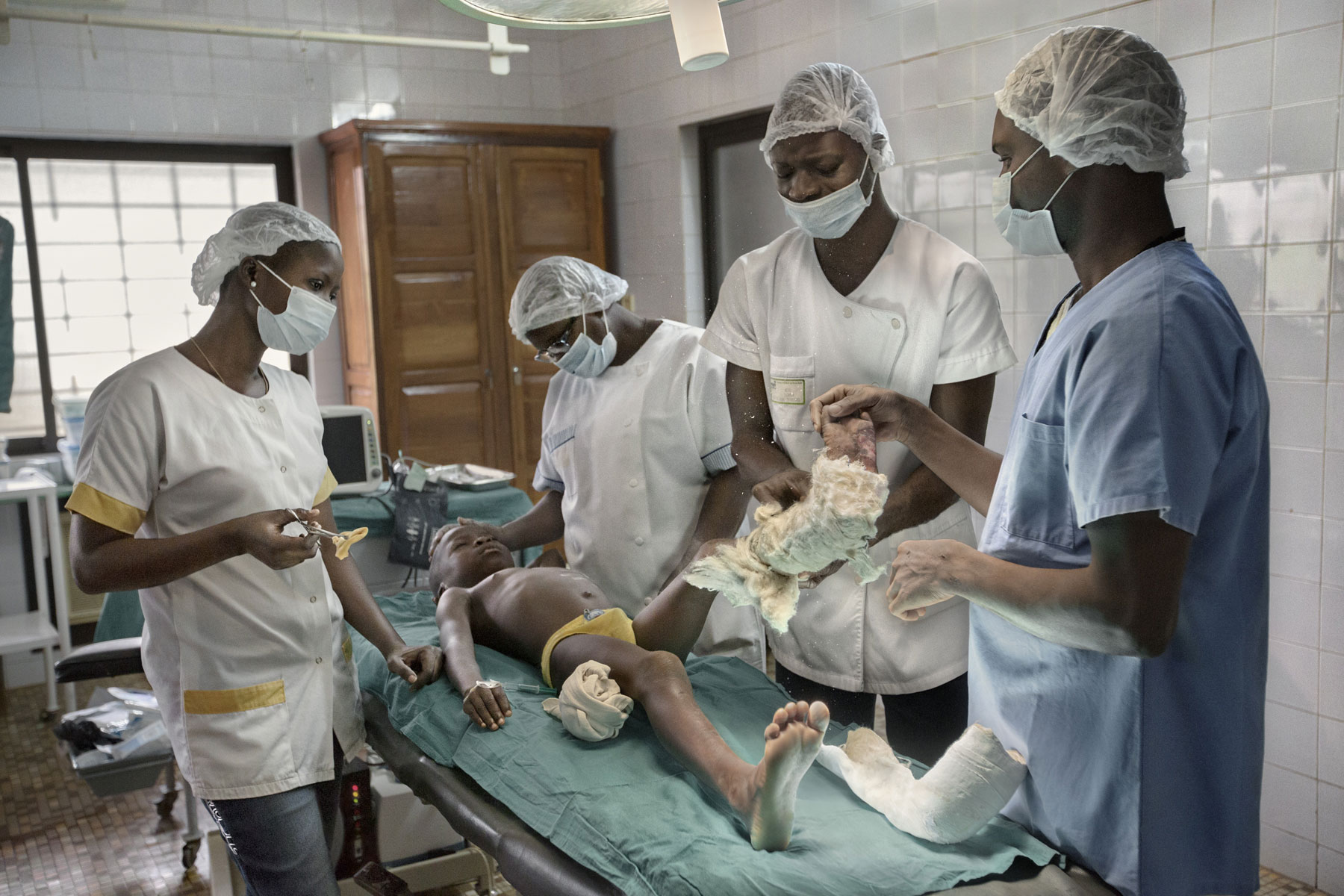
Preparing for an operation. Missionary Julia Aguiar is in charge of Gbemontin Hospital and was a pioneer in buruli ulcer surgery. One day a week she operates on an average of 50 patients.
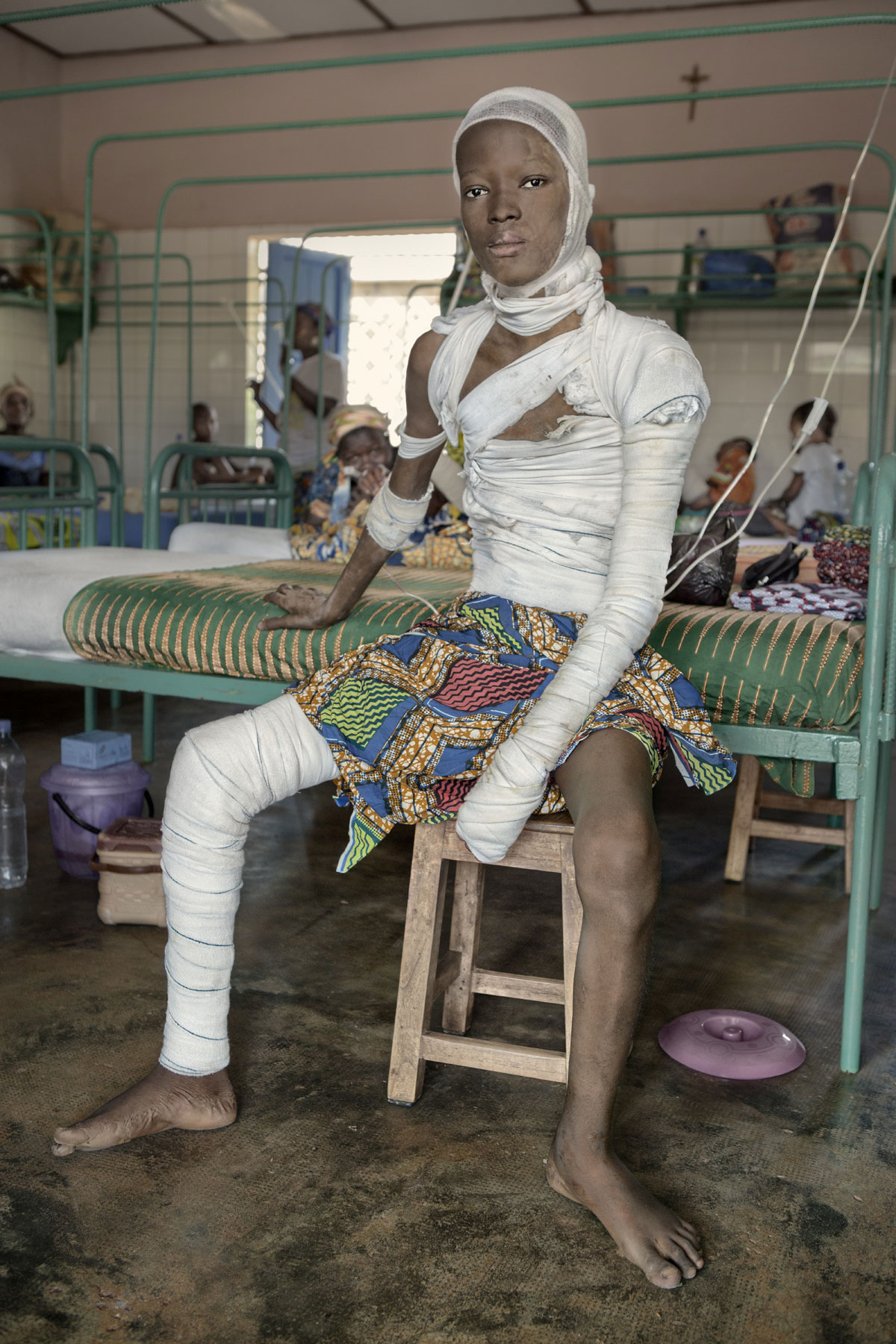
Attingly Michael, aged seventeen, suffered burns on 80% of his body after tripping over a pan of boiling palm oil one night. He’s recovering from one of the many skin tissue regenerating operations he’ll have to undergo in one of the wards at Gbenmontin Hospital, in Zagnanado, along with the 29 other patients he shares his room with.

Felicien recovers from his buruli ulcer operation in his room at the Davougon former leper colony. The beds have frames above them for fixing and elevating limbs to prevent inflammation setting.

Felicien recovers from his buruli ulcer operation in his room at the Davougon former leper colony. The beds have frames above them for fixing and elevating limbs to prevent inflammation setting.
Didier Agossadou, who heads a government plan set up specifically for this purpose, the National Programme for Fighting Buruli Ulcer, tells how 80% of cases picked up in the early stage – category I – can be cured:
“Early diagnosis and treatment with antibiotics has been really effective, even reducing the net morbidity rate associated with the disease in recent years. If it’s diagnosed at the advanced stage (category III) or treatment starts toolate, the result is lengthy hospital stays, which are costly for both patients and the government, plus there is a 25% risk of permanent side effects – shortening of limbs leading to reduced mobility. That’s why early detection is so important, to prevent people suffering from these irreversible injuries”.
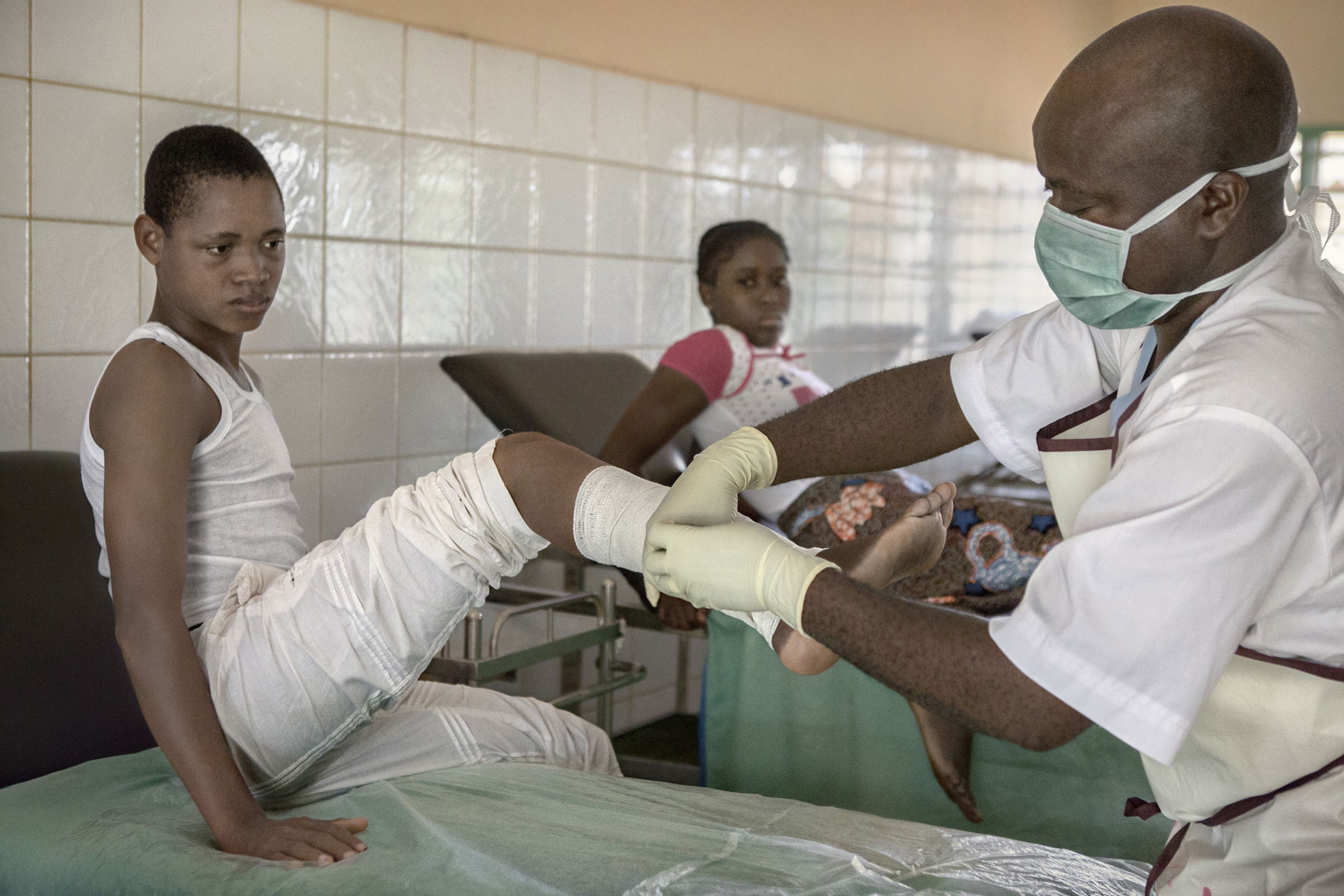
Treatment room at Lalo Commune Health Centre.

Sohinnou Estelle is having a splint fitted so she can stretch her hand and arm better. This procedure is part of the treatment given for buruli ulcer at the Lalo Commune Health Centre.
Africa’s skin. Rehabilitation.
Photography and video
Ana Palacios
With the collaboration of
DKV Health Insurance and Anesvad

Rehabilitation room at Gbemontin Hospital. One of the consequences of advanced stage buruli ulcer is reduced movement in the arms or legs, requiring daily stretching to recover limb mobility.
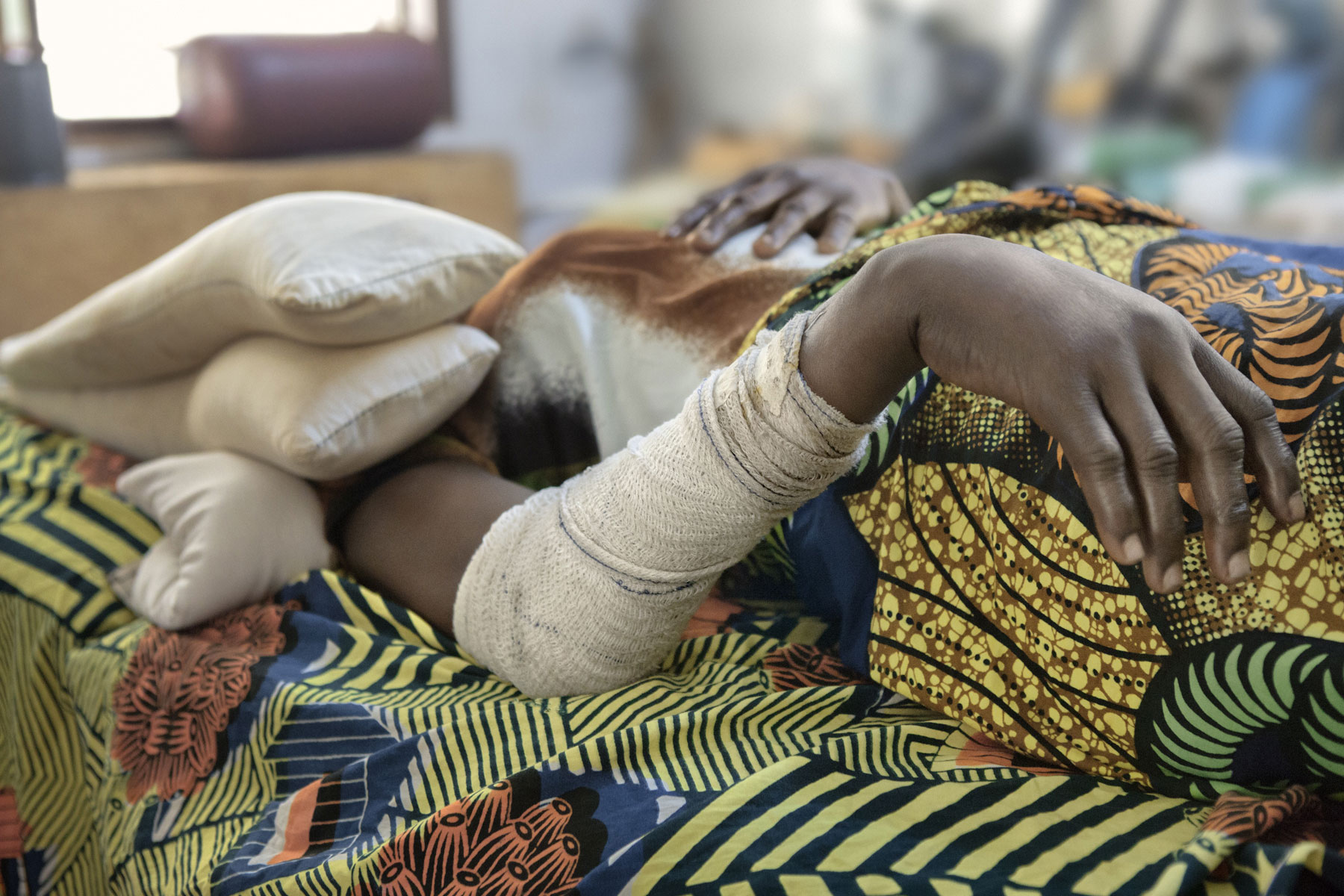
A patient undergoes physiotherapy in the rehabilitation room at Lalo Commune Health Centre in Benin, which specialises in the treatment of skin diseases.

Assogba Justin undergoes rehabilitation with a traction machine in the physiotherapy room at Lalo Commune Health Centre in Benin, which specializes in the treatment of skin diseases.



XL Semanal – Marcados a flor de piel (Inequality is Skin Deep). February 28th 2016
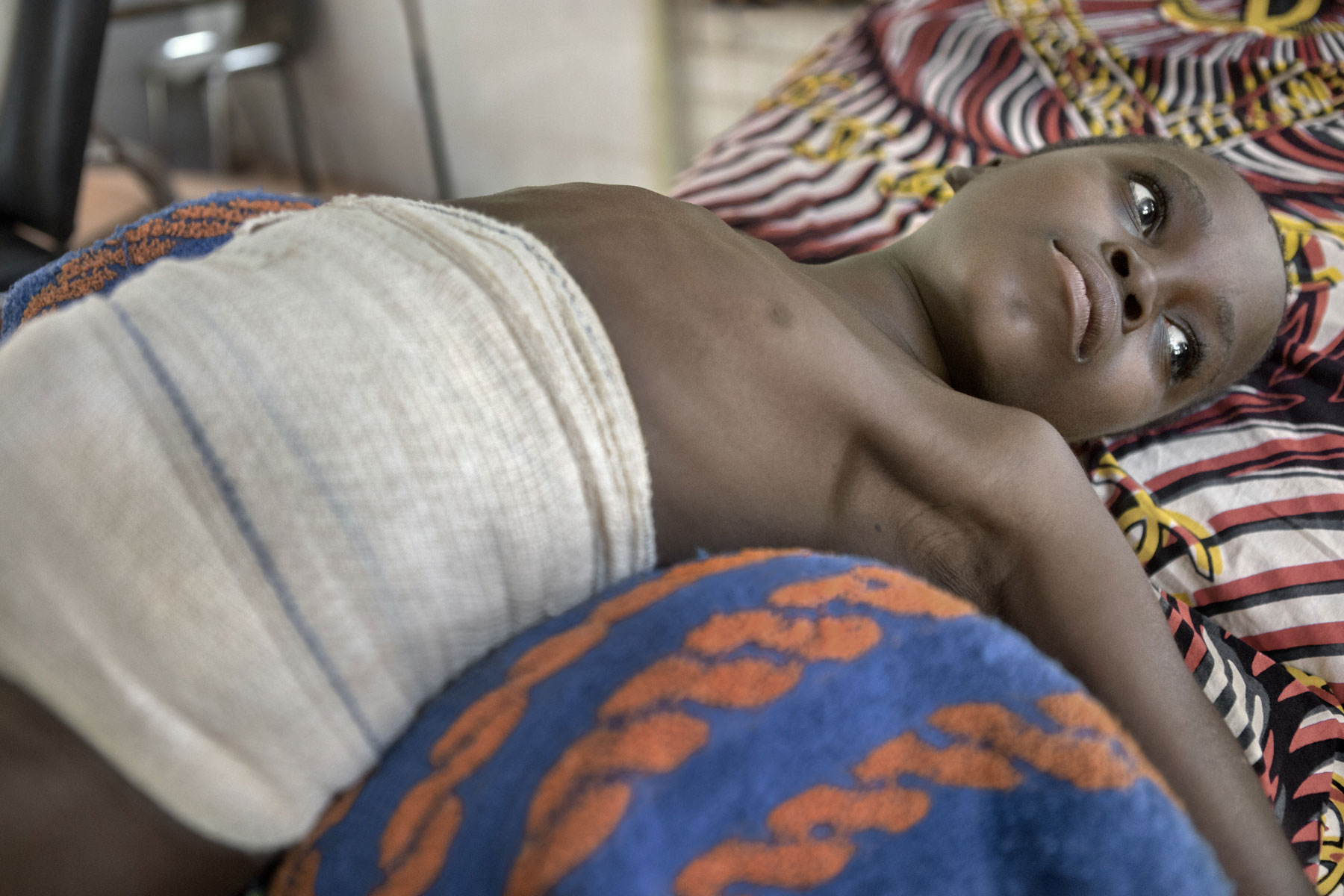
Physiotherapy room at Lalo Commune Health Centre.

Physiotherapy room at Lalo Commune Health Centre.

The former Davougon leper colony has a children’s schoolroom for inpatients that’s also used for informal educational activities.

Elpais.es – Desigualdad tatuada en la piel (Inequality is Skin Deep). February 29th, 2016

Freud Lokossou goes to class every day. The average hospital stay for patients with skin diseases is thirty days. The classroom in Gbenmontin Hospital caters for child inpatients of all ages so they don’t miss out on their schooling.

Freud Lokossou goes to class every day. The average hospital stay for patients with skin diseases is thirty days. The classroom in Gbenmontin Hospital caters for child inpatients of all ages so they don’t miss out on their schooling.

At the hottest time of day, Gbemontin Hospital patients shelter in the shady hospital corridors for hours.



Professional Photographer – Showing Hope. May, 2017

Afternoon playtime at Gbemontin Hospital. Rachelle has had the bandage on her foot removed so the wound can be examined and the same splint reused; for the time being she’s been told to rest.
The central aim of government and supporting health partners is to eradicate Neglected Tropical Diseases, especially Buruli ulcer in Benin, where patchymedical care and misinformation mean that the disease is much more widespread. The goal is to eradicate leprosy and control Buruli ulcer, working in line with WHO targets and the Sustainable Development Goals, which aim to “eliminate Neglected Tropical Diseases” by 2030.
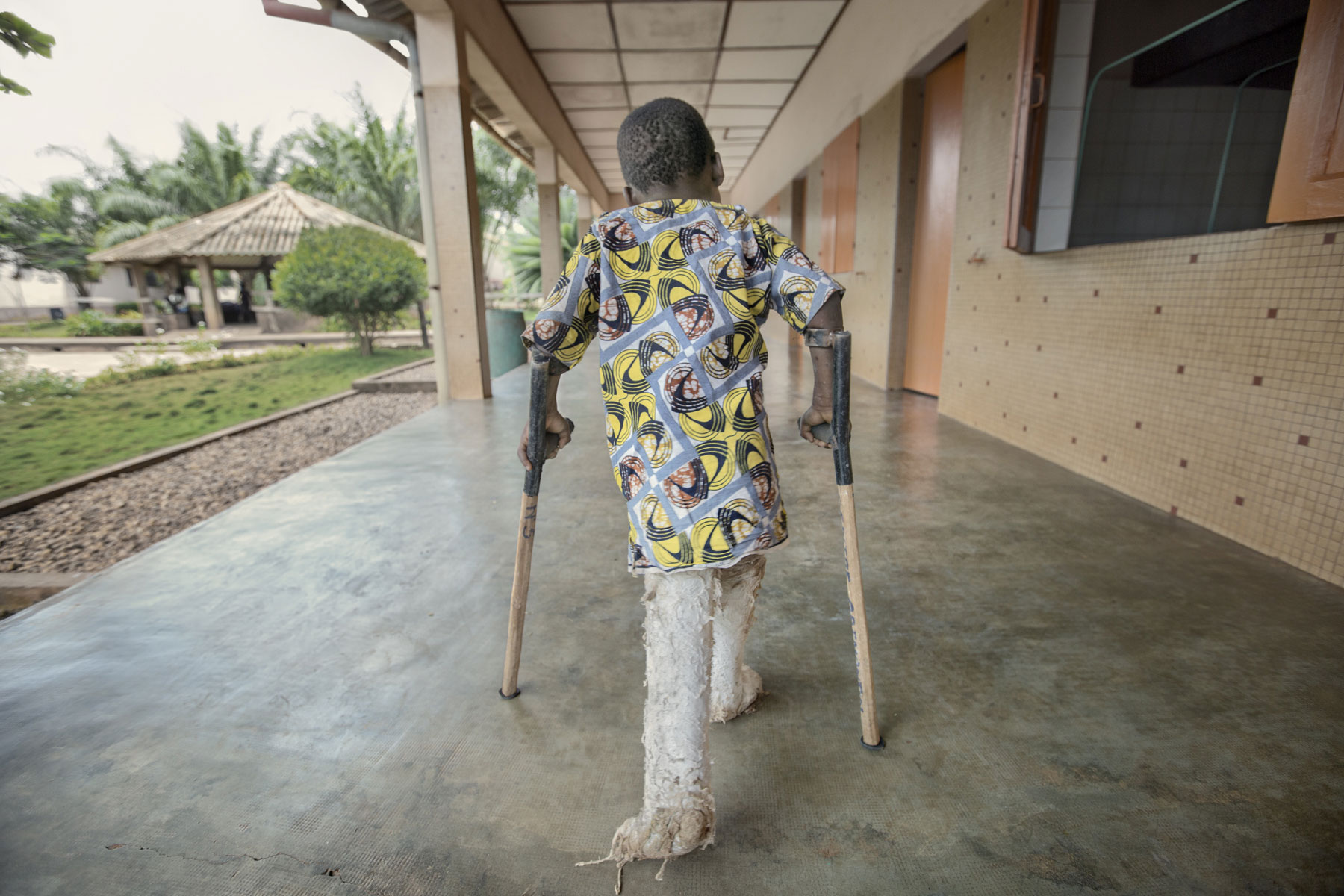
Four-year old Marius Agbosuno learns to walk using his new crutches. He’s been in hospital for three months. His mother had to leave his grandparents Serafin and Louise in charge of his care, as she couldn’t leave her job for such a long period.

Four-year old Marius Agbosuno learns to walk using his new crutches. He’s been in hospital for three months. His mother had to leave his grandparents Serafin and Louise in charge of his care, as she couldn’t leave her job for such a long period.
La piel de África
Photography
Ana Palacios
If you have made it this far and you enjoyed it, you should know there is an exhibition available of this project.
Please, feel free to contact me@ana-palacios.com for further details.
La habitación de juegos
Galería Luis Burgos. PhotoEspaña. Madrid.

The Skin of Africa
Granada Eclipsa Festival. Parque Tecnológico de la Salud. Granada.

The Skin of Africa
Sala de Exposiciones de la casa de la Cultura “Ca Don José”. Canals, Valencia.

The Skin of Africa
Imaginaria photo festival. Castellón.
The Skin of Africa
Hospital Viamed Los Manzanos. Logroño.

The Skin of Africa
Denia Hospital. Denia (Alicante).